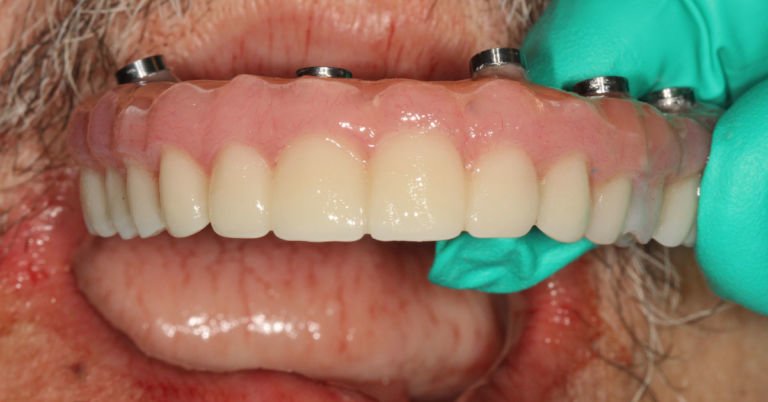
How to Cement Ti-Bases to Zirconia Crowns Using Microetching and Resin Cement
I do a lot of implant dentistry and a big portion of that is digitally produced! There’s a certain amount of excitement surrounding creating something from scratch. Whether it’s baking a loaf of bread, making a bowl from clay, or fabricating a dental restoration… we are makers. Dentists can create amazing things in their offices and dental laboratories!

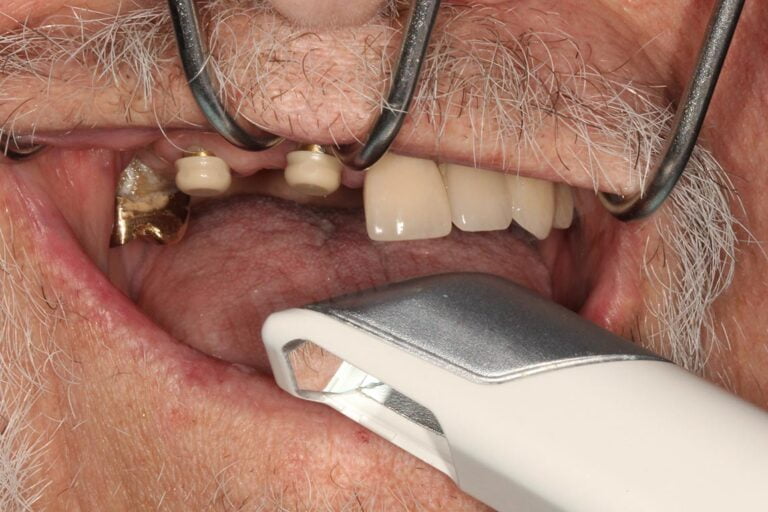
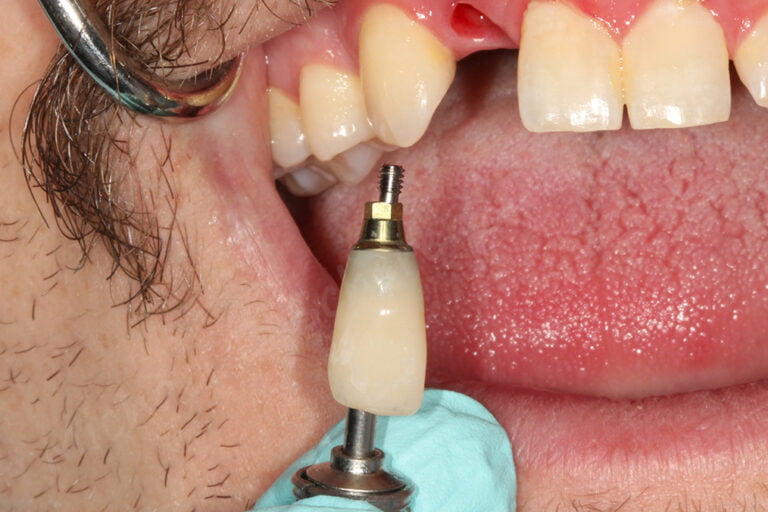
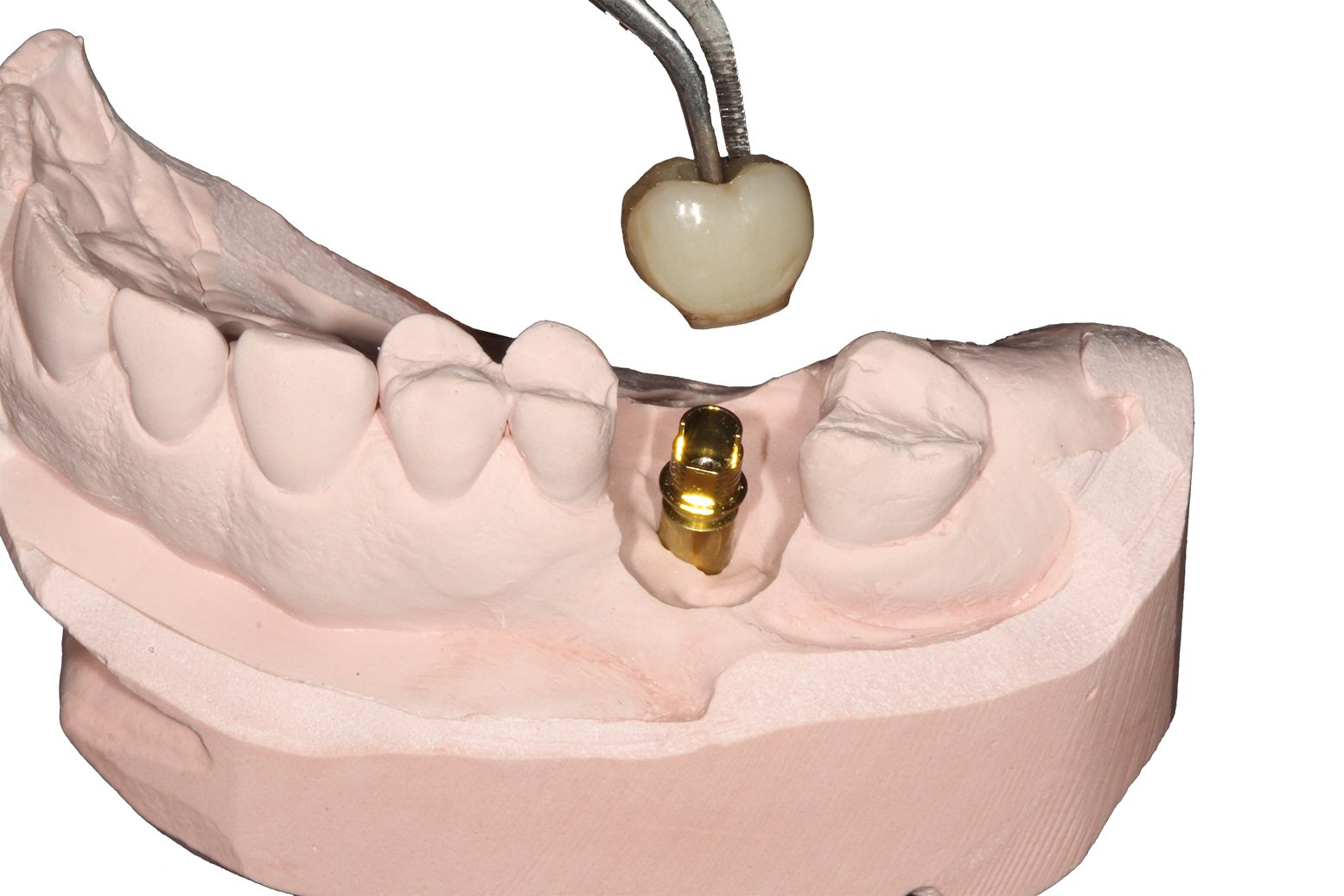
When it comes to screw-retained restorations on dental implants, we have a simple choice… custom abutment or ti-base. While there are merits to using both approaches, this article is aimed at working with the latter. A ti-base is essentially a titanium abutment that has one fit size. In digital software, such as 3Shape or exocad, the clinician/technician can design a crown that can be cemented on top of the ti-base, effectively turning a singular crown made from Zirconia, eMax, or even metal like a PFM or all-gold crown into a screw-retained crown. It sometimes feels like magic!
The biggest challenging is ensuring that the designed crown fits well enough and the metal portion is jointed to the ceramic portion strong enough that the crown stays on top of the metal portion that joints to the dental implant. Debonding of the crown from the ti-base is something we all want to avoid… thankfully it doesn’t happen very often, but when it does, it’s a pain! What went wrong? Did we follow a smart protocol for cementing the crown?

There are many companies in dentistry that manufacture ti-bases and they come in several different designs but typically ti-bases are cylindrical in shape and are either sandblasted or are machined. One ti-base is from the company NT Trading, they have a unique geometry with a tiny little notch that helps position the final crown during cementation protocols. The biggest drawback is that they are not sandblasted or roughened prior to fitting the crown. Turns out surface treatment on ti-bases is critical and has been studied in the literature. Check out this recent article describing retention of ti-bases and surface treatments. Kemarly K. Effect of Various Surface Treatments on Ti-Base Coping Retention. Oper Dent. 2020 Feb (https://www.ncbi.nlm.nih.gov/pubmed/32053453)

Another company is DESS, they have unique features such as yellow anodized surface for esthetics and their ti-bases are pre-blasted so microetching by the clinician or technician isn’t necessary nor recommended. That’s awesome! We will look at their ti-bases in other posts, but let’s talk about cementing crowns to non-blasted ti-bases in this post.

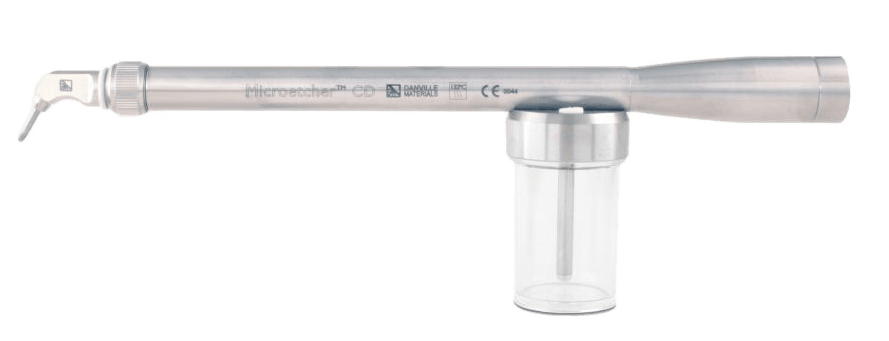
Ensuring that the ti-base has been abraded correctly, I recommend using a microetcher that is simple to use and is effective for many purposes. I like the Zest Dental Solutions / Danville Microetcher. It comes in two different styles: 1) the Microetcher II/IIA which hooks up via a quick disconnect hard line to my laboratory or dental unit or 2) the Microetcher CD which can plug directly into your dental handpiece unit in your treatment room. I prefer the Microetcher IIA for my laboratory and the Microetcher CD for using in chairside situations.
I have come up with some tips for cementing ti-bases. Important to understand is that this is some general recommendations based upon my empirical experience and from my understanding of the literature.
Dr. Scherer’s tips for cementing ti-bases:
- Monolithic Zirconia crown has been properly designed, milled, polished (or glazed) and internal surface has been microetched properly using aluminum oxide grit of choosing. I prefer 50um although some others prefer larger grit sizes.
- Ti-base chosen for the system is a straight, minimally tapered cylinder of moderate to tall height and has been roughened with aluminum oxide grit of choosing. I prefer 50um although some others prefer larger grit sizes.
- Crown fits on ti-base moderately tight but seats all the way. Passive crowns on ti-bases feels great during lab procedures but may result in increased debonding rates.
- Resin cement and matched primer surface treatment used on zirconia crown and/or ti-base. Some resin cements have a primer for metal alloy, others do not. I prefer using a very simple resin cement like Panavia v5 since I get very good bonding but with less primer steps needed. This system only has a ceramic primer and is properly indicated for cementing prosthetic crowns to implant abutments.
- Dry the ti-base and zirconia crown fully! I work in a laboratory environment that has lots of dust floating around. Make sure you properly clean and dry your components prior to using resin cement.
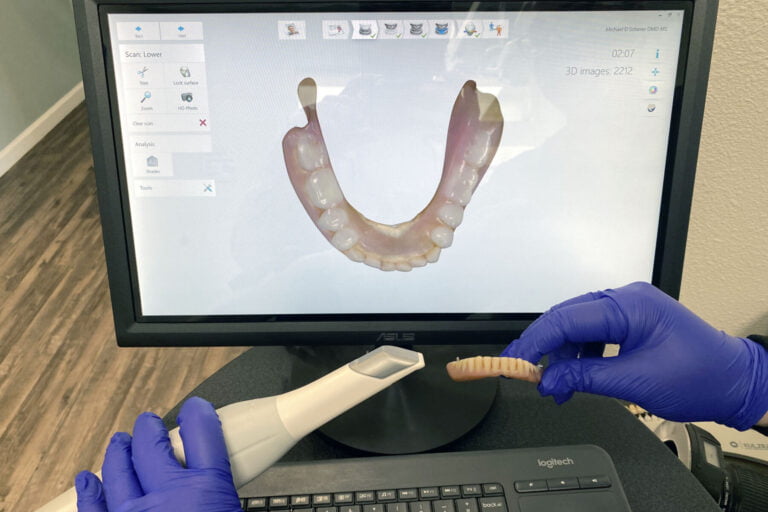
- Cement the ti-base on the printed or stone model! While this depends on how tight your tolerance between your zirconia and ti-base are and the design of the ti-base itself, but cementing on the printed or stone model is the safe and predictable approach.
- Filling your screw-channels with cotton balls, not PTFE! This makes for very simple clean-up of excess cement. I just grab an explorer and tug the cotton out, much easier to remove than PTFE tape.
- Partially unscrew the ti-base right before cementing. I personally like cementing the crown over the ti-base, cleaning the screw channel, then tightening down the screw the rest of the way. This method is is very predictable in my hands for some reason! If you like it tightened down all the way at first or prefer not using a model, no worries… that’s your call!!
- Light cure fully but leave ti-base sitting over night prior to removing from the model. Even though I’m using dual-cured resin cement and can be light cured, there’s a portion of it that doesn’t get exposed to the light. I just like it when the cement sets up overnight and remains undisturbed during the complete polymerization cycle.
- Polish zirconia near ti-base after cementing. A nicely polished and smooth subgingival zirconia surface makes for happy tissues. I use laboratory polishing discs from Pearson Dental.
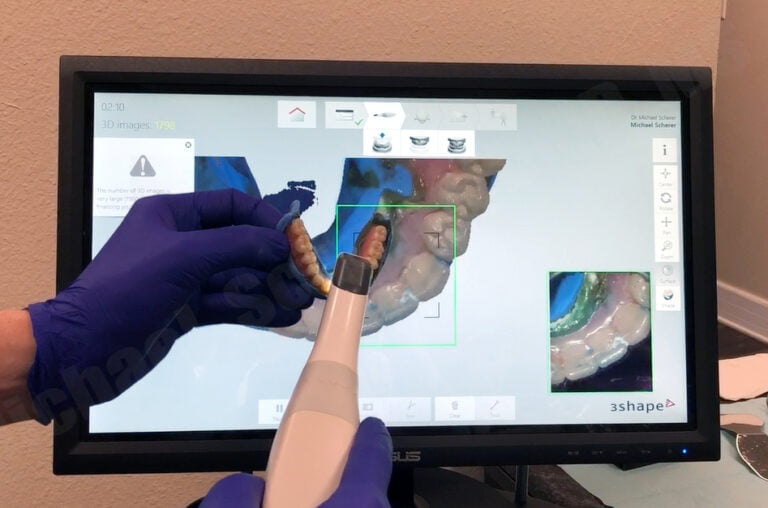
I put together this video which illustrates the step-by-step protocols that I use in my dental office to make routine screw-retained crowns, check it out:
Interested in learning more about digital dentistry and step-by-step videos on clinical and laboratory techniques? Check out the online course www.LearnDental3D.com

Dr. Michael Scherer, DMD, MS
Dr. Michael Scherer is an Assistant Clinical Professor at Loma Linda University, a Clinical Instructor at University of Nevada – Las Vegas. He is a fellow of the American College of Prosthodontists, has published articles, books, and in-person and online courses related to implant dentistry, clinical prosthodontics, and digital technology with a special emphasis on full-arch reconstruction.